Over 30 years of anarchist writing from Ireland listed under hundreds of topics
In a State of Emergencies - Healthcare Workers Under Pressure
As the number of patients reached a record high in recent days, healthcare workers in Emergency Departments (ED) in the country strive to maintain some acceptable standard of care delivery for patients. However nurses and doctors admit they are swamped and feel that current activity is unsustainable if the safety of patients is to be maintained. In some of the bigger centres in the country the huge backlog has created the situation where there is standing room only for ED patients. There is agreement among healthcare workers that the result of the over-crowding can only be increased morbidity and mortality for those requiring emergency treatment.
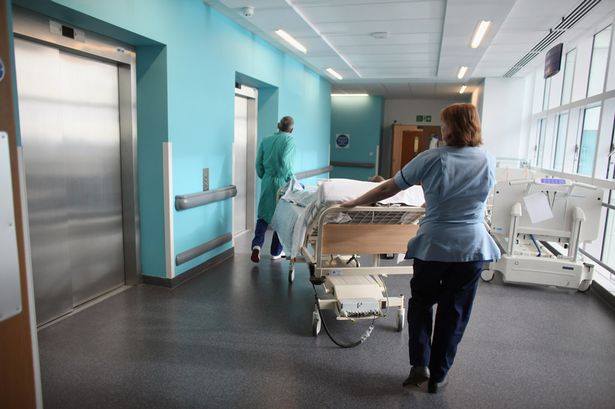
As the head of the newly convened Emergency Department Task force, Dr. Tony O’Connell jumps ship, the minister for health Leo Varadkar (just back from holidays) admits he is “sick to death” of the crisis, though not actually as sick as those who have waited for days on chairs and hospital awaiting admission to a ward. The minister concurs that there are too few community based beds to accommodate patients who are fit for discharge from the acute hospital setting, but as of yet has not revealed his plan to provide such beds. It is in the plan however to increase bed capacity in the acute setting to relieve the pressure on EDs. While this will provide a very short term solution to reducing numbers on trolleys – leading to more positive media reporting, it will be like putting a band aid on to try and stop a massive haemorrhage.
There is no talk of increasing the numbers of nurses, which were significantly reduced during the Croke Park/Haddington Road debacle, to cater for the extra patient numbers. The health and safety of both patients and nurses will be greatly impacted by this move. Nurses who are already under pressure to provide the highest standards of care on ever decreasing budgets understand that patients admitted into already full capacity wards will suffer increased health risks. Risks will involve less direct attention from nurses, greater infection control risks due to overcrowding, delayed delivery of care and generally degraded quality of care. This clearly is no solution.
In recent months we have seen nurses organise to resist a 50% increase in their professional retention fee, charged by their regulatory body Nursing and Midwifery Bord of Ireland (NMBI). This body is responsible for overseeing standards and nursing/midwifery practices in the State, and convenes Fitness to Practice hearings to establish if nurses have carried out their expected role to the set standards. How are nurses expected to meet these standards of patient care realistically when patient-nurse ratios will far exceed the accepted safe level. Therefore now not only are patients at increased health risk, nurses are risk too – of losing their job.
The Minister for Health, the HSE management don't have the luxury of time to take a long hard look at this crisis – they need to act, and act fast. Though this crisis is hardly new. But patient safety must be to the forefront of any plan they agree upon. Provide the nursing home beds, employ more nurses and healthcare assistants. Bailout the hospitals and the people for a change.